Hemolysis is the breakdown of red blood cells (RBC). A substance that causes hemolysis is a hemolysin. Brown (1919) introduced three terms alpha, beta and gamma to indicate three types of streptococci based on haemolytic reactions observed on blood agar plates.
Beta-hemolytic Streptococci
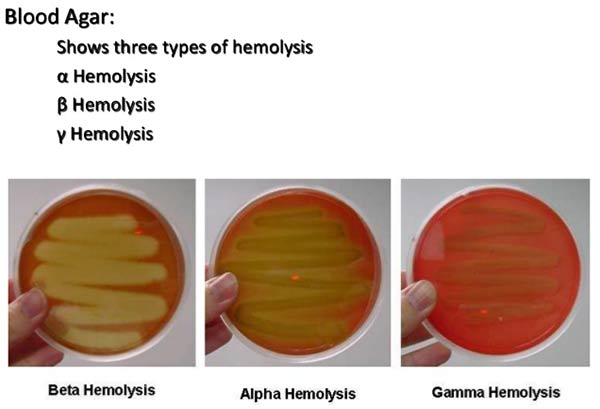
Beta-hemolysis (β-hemolysis) is associated with complete lysis of red cells surrounding the colony. Beta hemolysis is caused by two hemolysins O and S; the former is inactive in the presence of oxygen. Thus, stabbing of the plate increases the intensity of the hemolysis reaction. S is an oxygen-stable cytotoxin.
It exhibit a wide zone (2-4 mm wide). Beta hemolysis is more marked when the plate has been incubated anaerobically. They are generally commensals of throat and causes opportunistic infections.
Examples: Streptococcus pyogenes, or Group A beta-hemolytic Strep (GAS).
Weakly beta-hemolytic species: Streptococcus agalactiae, Clostridium perfringens, Listeria monocytogenes
Alpha-hemolytic Streptococci
Alpha-hemolysis (α-hemolysis) is a partial or “green” hemolysis associated with reduction of red cell hemoglobin. Alpha hemolysis is caused by hydrogen peroxide produced by the bacterium, oxidizing hemoglobin to green methemoglobin.
It exhibit incomplete haemolysis with 1-2 mm wide. Persistence of some unhaemolysed RBC’s can be seen microscopically.
Examples: Streptococcus pneumoniae and a group of oral streptococci (Streptococcus viridans or viridans streptococci)
Gamma-hemolytic (Non-haemolytic) Streptococci
Colonies show neither typical alpha nor beta haemolysis. There may be, however, slight discoloration in the medium. The streptococci included in this group are usually not pathogenic.
Examples: Enterococcus faecalis (formerly called “Group D Strep”)

He were mention gamma as not for all media gives no hemolysis but some of them gives too slightly partial hemolysis. Thats why he were prefer gamma among of his mentioned hemolysis.
Why did Brown (1919) mention gamma haemolysis when there was no haemolysis??
Hi and thank for your info can you help me gather some info on “alpha prime haemolysis”?
Small zone of intact erythrocytes immediately adjacent to bacterial colonies with complete hemolysis sorrounding yhe zone of intact erythrocytes
thanks for you
please can you give me any information for streptococcus mutans.(isolation .charactrestic. biochemical test . habitat .pathogenicity )
Thanks You make this articule very good and nice.Normally i know this but not all streptococcus viridans that is group Alpha hemolisis really I forget.Super and nice.Good job.
Best regards
I am microbiologist now am taking my MSc in microbiology from Addis ababa University, any one interested to contact me am voluntere to discuss specially in bacterial identification and isolation
what are the other bacteria that bring outs those three hemolysis aside from Streptococcus?
Hi, I was diagnosed with beta after doing a throat culture in my biology class but when I went to the doctor for confirmation of strep, it came back negative. Also I have been having a painful throat everyday all day for over two years now. Had an MRI with a ENT doctor and said everything looked fine. I know something is wrong and my beta agar test proved it but for some reason doctors are unable to help.
Your test proves nothing!
S. aureus is a very a common bacterium found in the throat.
I suggest you take a microbiology course.
Your throat could be sore for a number of reasons: post-nasal drip, allergies, poor diet, or poor hygienic habits (brush, floss, and use a tongue scraper twice a day), and have a dental cleaning every 4-6 months.
Bacteria are our friends. We cannot live without them!!
Thank you all for discussion of these basic topics.Being a pathologist not mch in touch with micro.. But nice refreshment.. Would be looking forward to all kinds of discussions in micro.. Basics as well as advanced research.